Cauda Equina Syndrome Medical Malpractice Attorneys in Pennsylvania
Contact Frischman & Rizza Today
Frischman & Rizza, P.C.
Quick Facts
CES can be caused by any condition that pinches or compresses the nerve roots in the lumbar spine.
CES typically results in weakness and numbness from the waist down.
CES is a medical emergency.
CAUDA EQUINA SYNDROME
Cauda Equina Syndrome (CES) is a rare, yet potentially debilitating spinal condition.
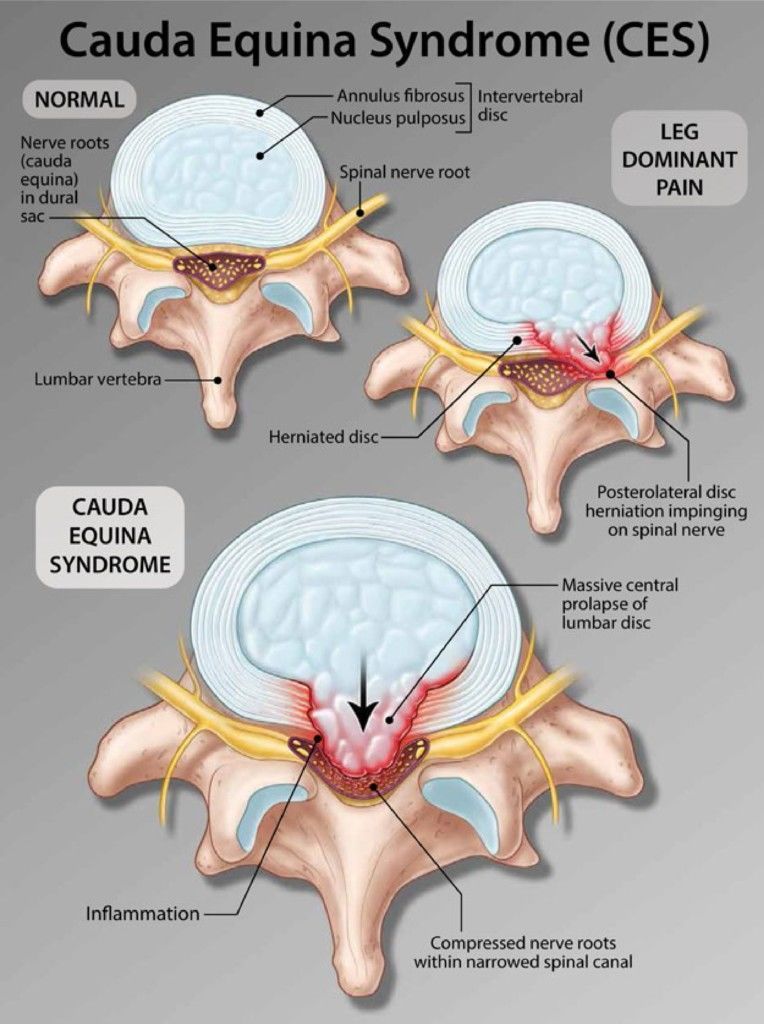
The Cauda Equine consists of approximately 10 pairs of nerve roots that are located at the end of the spinal cord in the lumbosacral region. These nerves, which get their name because they look like a horse’s tail (see image below), are responsible for sending and receiving messages to and from the legs, feet and pelvic region. When the nerve roots that make up the cauda equina become pinched or compressed, weakness, numbness and potentially paralysis from the waist down along with the loss of bladder and bowel control will occur.
Diagnosing CES can pose a challenge as its symptoms, such as low back pain, vary and can develop over time. Also, low back pain, even of a severe magnitude, impacts many people of all ages, and is often due to much less serious conditions.
For those patients who become afflicted by CES, the timely diagnosis and initiation of appropriate treatment is essential to preventing debilitating and permanent spinal cord damage.
Have you been injured?
Contact a Pittsburgh Personal Injury Attorney at Frischman & Rizza for a free case evaluation.
Call Us On
Cauda Equina Syndrome Causes
CES can occur in patients of all genders and ages. However, it most often occurs in adult patients and is commonly caused by:
- A severe ruptured disc in the lumbar spine.
- The narrowing of the spinal canal, which is known as spinal stenosis.
- Spinal infections and/or hemorrhage.
- Violent trauma and injury to the lower back (auto accident, penetrating trauma).
- Spinal tumors and cysts.
- Birth defects, such as an abnormal connection between blood vessels (arteriovenous malformations).
- Post-lumbar spine surgery complications.
- Spinal blocks.
CES Symptoms
Because CES symptoms vary from patient-to-patient and mimic other much less serious conditions, CES can represent a challenge to diagnose.
CES can be of an acute onset where the patient experiences the rapid development of severe low back pain that is accompanied by the corresponding loss of bladder and bowel function. In those situations when CES occurs acutely, the patient typically will develop sensory and motor deficits in the lower body within 24 hours. Conversely, CES can develop progressively over the course of days, weeks and even months. With the gradual onset of CES, the patient often experiences the partial or intermittent loss of bladder and bowel function along with recurring low back pain and corresponding muscle weakness and/or numbness.
Cauda Equina Syndrome must be considered anytime a patient presents to an ER or healthcare provider complaining of the sudden onset of extreme low back pain and any of the following symptoms:
- Motor weakness, sensory loss or pain in one or both legs.
- Saddle anesthesia (this is where the patient has limited or no feeling in those portions of the body where he or she would sit on a saddle to ride a horse).
- Recent onset of bladder or bowel dysfunction.
- Bowel incontinence.
- Loss of reflexes in the rectum and/or the legs.
If CES is suspected, emergent MRI or myelogram imaging of the lumbar spine is necessary to assess the patient for compression on the nerve roots that make-up the cauda equina.
Treatment
CES is a surgical emergency that involves removing the source of the compression on the cauda equina. If left undiagnosed and/or untreated, CES will cause permanent paralysis from the waist down and incontinence. Typically, those patients who undergo surgery within 48 hours of the onset of CES symptoms, have a more favorable outcome. The failure to suspect CES, to recognize that the patient’s neurologic condition is worsening, to order appropriate imaging tests for suspected CES or delays in performing surgery are common causes of CES related medical malpractice.
Frischman & Rizza, P.C.
In Western PA Since 1992
Injured & Need an Attorney? Call Craig and Bernie!
- The Call Is Free
- The Consultation is Free
- We Don’t Charge A Penny Unless We Win Your Case!